Recurring Migraine Symptoms: Why Patterns Change

Recurring Migraine Symptoms: Why They Don’t Follow a Pattern
Migraines are often described as a recurring condition, but anyone who lives with them knows that recurrence doesn’t always look the same. If you suffer from recurring migraine symptoms, you might notice that some episodes feel incredibly intense, while others are much milder. Some may appear frequently over a few short weeks, while others only strike after long, unpredictable gaps.
This variation is one of the main reasons people struggle to understand what their symptoms mean, whether their condition has changed and if their current treatment plan is actually working.
This article focuses on why migraine patterns often lack consistency, what that variation usually indicates and how you can take control of your health without falling into a cycle of unnecessary medical anxiety.
Why Recurring Migraine Symptoms Can Look Different Each Time
When dealing with a chronic condition, it is natural to look for a predictable cycle. However, migraine symptoms are not fixed. Even within the exact same person, consecutive episodes can drastically differ in several ways:
Duration:
One attack might resolve in four hours, while the next lasts for three days.
Intensity:
You may experience a mild, dull throb one month and a debilitating, sharp pain the next.
Associated Sensations:
Symptoms like severe light sensitivity, nausea, visual auras, or intense fatigue might be present during one episode and completely absent the next.
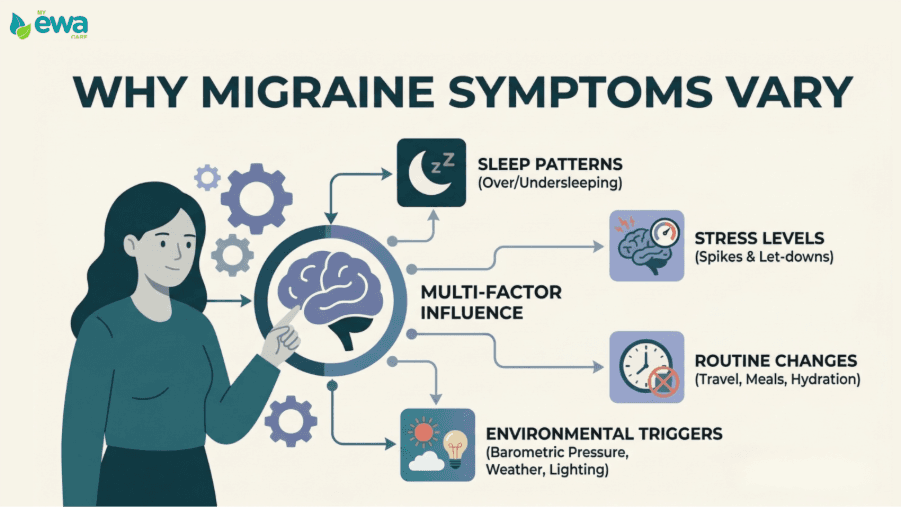
This inconsistency happens because migraines are rarely triggered by just one thing. Instead, they are influenced by multiple factors at once, including:
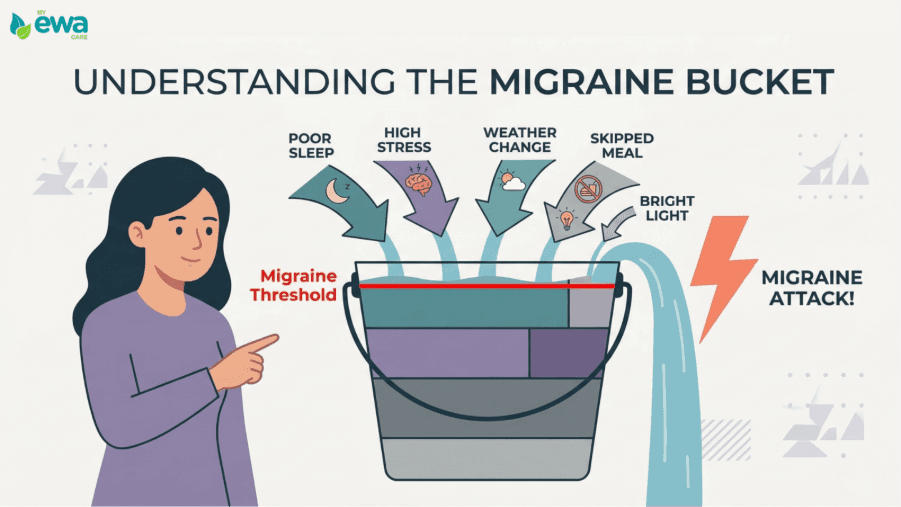
Sleep Patterns:
Both lack of sleep and oversleeping can shift how a migraine presents.
Stress Levels:
Spikes in daily stress, or even the sudden relaxation after a stressful period (known as a "let-down" migraine), can alter your symptoms.
Routine Changes:
Skipping meals, dehydration, or traveling across time zones.
Environmental Triggers:
Sudden shifts in barometric pressure, weather changes, or bright artificial lighting.
When these underlying lifestyle and environmental factors shift, your physical symptoms can change right alongside them. As a result, expecting recurring migraines to follow a highly predictable format often leads to confusion and frustration.
When Recurring Migraine Symptoms Change Unexpectedly
When you do not know what to expect from your own body, it can take a mental toll. People commonly feel unsure or anxious about their condition when:
Migraines return after a symptom-free period: You may have thought you outgrew them or found the perfect cure, only for the pain to return unexpectedly.
The pain feels different from previous episodes: A shift from unilateral (one-sided) pain to tension at the back of the neck can feel alarming.
Known triggers don’t seem relevant anymore: A food or environment that used to guarantee a migraine suddenly has no effect, while new triggers seem to emerge out of nowhere.
Relief is temporary rather than sustained: Medications that used to stop an attack in its tracks may suddenly only take the edge off.
These shifting changes often raise difficult questions about whether something new is developing medically, or whether earlier assumptions about the condition were incomplete.
Why Inconsistency Doesn’t Always Mean Progression
A very common concern among patients is that changing symptoms automatically indicate that their condition is worsening. It is important to know that in many cases, variation reflects fluctuating daily influences rather than a true, long-term progression of the disease.
For example, consider the following shifting patterns:
A single, more intense episode doesn’t always mean increased frequency is ahead.
A period of reduced pain doesn’t always mean the migraines are permanently resolving.
New accompanying symptoms (like suddenly experiencing dizziness or nausea) don’t always point to a brand-new neurological issue.
Understanding that inconsistency is a built-in feature of recurring migraines helps reduce unnecessary worry and panic when your patterns inevitably shift.
When Additional Steps Don’t Always Explain the Pattern
In response to changing recurring migraines, people sometimes pursue further medical steps like repeat MRI scans, new specialists, or advanced testing expecting clear, definitive answers. However, when those steps don’t directly explain the symptom patterns, they can unfortunately add more questions instead.
This frustrating cycle often happens when:
Findings don’t clearly connect to daily experience: A scan might come back completely clear, which is good news, but it doesn't explain why you are in pain.
Results remain unchanged despite symptom variation: Bloodwork might look identical to last year, even though your migraines feel twice as bad this month.
Follow-ups repeat without offering new insight: You might find yourself having the same conversation with your doctor without adjusting the actual treatment strategy.
Without absolute clarity on what a medical step or test is meant to explain, repetition can increase uncertainty rather than resolve it.
Understanding How Healthcare Costs Build Gradually
Migraine-related healthcare costs often accumulate quietly. This financial drain happens through repeat clinic visits, repeated diagnostic investigations, or frequent medication changes that ultimately don’t alter your understanding of the root problem.
When medical steps are taken reactively without a clear goal, your effort and financial expense can increase rapidly without improving your clarity or your quality of life. Being incredibly clear with your medical team about what each step is meant to clarify helps avoid unnecessary repetition.
How Tracking Recurring Migraine Symptoms Can Add More Clarity
Instead of focusing only on putting a specific medical label on the condition, observing your personal patterns over time can be a much more useful and empowering strategy.
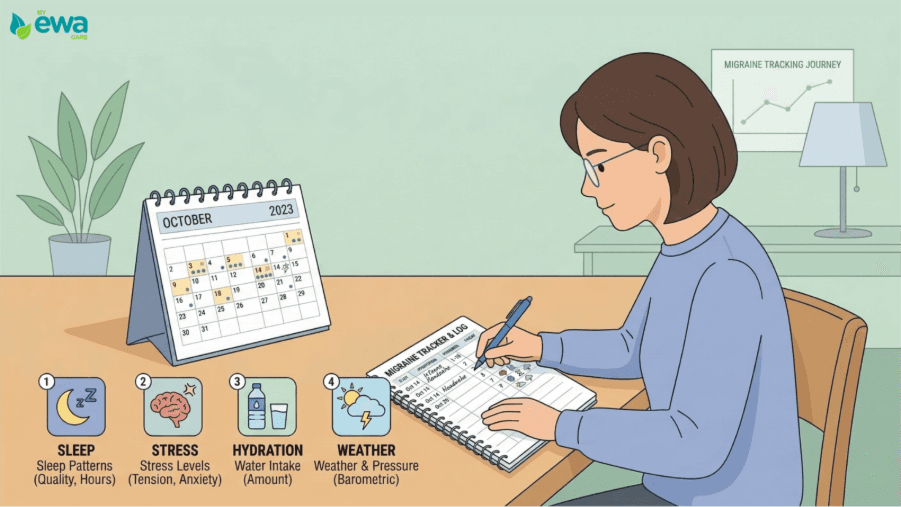
Tracking your daily habits provides concrete data. To get the best results, start tracking:
Frequency:
Exactly how many headache days are you having per month?
Duration:
Are the attacks lasting hours or days?
Possible Triggers:
Note your sleep quality, hydration, stress levels and weather changes.
Recovery Time:
How long does the postdrome (the "migraine hangover") last after the pain stops?
Tracking often provides significantly better insight into what influences your symptoms and what doesn’t. Bringing this organized information to your appointments can make future discussions with your doctor much more meaningful and actionable.
What to Ask When Migraine Symptoms Keep Changing
To avoid medical burnout and get the most out of your appointments, come prepared. Here are the best questions to ask your healthcare provider when your migraine symptoms keep changing:
What explains the specific variation I’m noticing right now?
What would this recommended test or step help confirm or rule out?
Is it reasonable to simply monitor these new patterns before taking immediate action?
What specific changes would indicate a real need to reassess my treatment plan?
These questions support clearer conversations, prevent unnecessary medical spending and help you make more confident healthcare decisions.
Key Takeaways for Recurring Migraine Symptoms
Recurring migraines can feel incredibly frustrating precisely because they refuse to follow a set, predictable pattern. Recognizing exactly why your symptoms vary from daily stress to shifting sleep schedules can help reduce your uncertainty and make your future treatment choices feel much more grounded.
If you are struggling to make sense of your changing symptoms, speak to a Care Manager for tailored guidance before you decide on your next steps.
Common Questions About Migraine Variation
Can an episode occur without any head pain?
Episodes without head pain, often called "silent migraines," involve sensory symptoms like visual disturbances, dizziness, or nausea without the actual throbbing ache. This type of variation is another reason why symptoms often feel like they lack a consistent format.
What is the expected duration of a single attack?
While duration varies, a typical episode lasts between 4 and 72 hours. When symptoms change and a single episode extends beyond 72 continuous hours, known as “status migrainosus” it represents a shift that requires medical intervention, even for those used to recurring patterns.
Why do attacks sometimes trigger after a stressful period end?
The sudden drop in stress hormones when a high-pressure situation resolve can initiate an episode. These "let-down migraines" often occur at the start of a weekend or vacation, making it difficult to connect the symptoms to an immediate, active trigger.
Does the recovery phase change depending on the episode?
The postdrome phase i.e the exhaustion and brain fog after the head pain subsides, it varies just as much as the attack itself. While recovery is sometimes immediate, fatigue and difficulty concentrating can linger for an additional 24 to 48 hours depending on how the specific episode influenced the body.
What specific changes indicate an emergency rather than normal variation?
While shifting patterns are common, certain changes indicate an emergency rather than fluctuating daily influences. A "thunderclap" headache (explosive pain that peaks within seconds), sudden numbness, confusion, or a headache accompanied by a fever require immediate medical care.